Our Foundations Podcast
Effectiveness of Adding a Mask Recommendation to Other Public Health Measures to Prevent SARS-CoV-2 Infection in Danish Mask Wearers
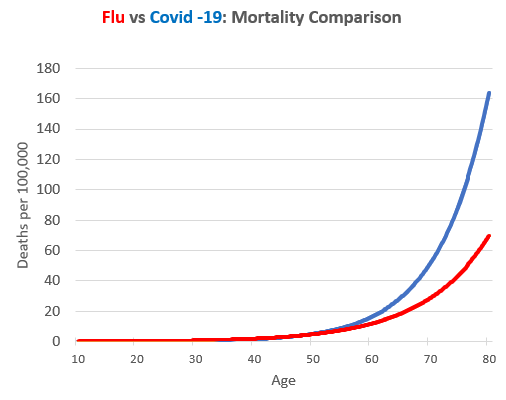
Corona virus mortality equals seasonal flu
94% of deaths in Bergamo were caused by transferring sick patients to nursing homes where they infected old people with weak immune systems
Doctors and hospitals worldwide were paid to declare deceased victims of Covid-19
Autopsies showed:
Fatalities almost all caused by serious pre-existing conditions
Almost all deaths were very old people
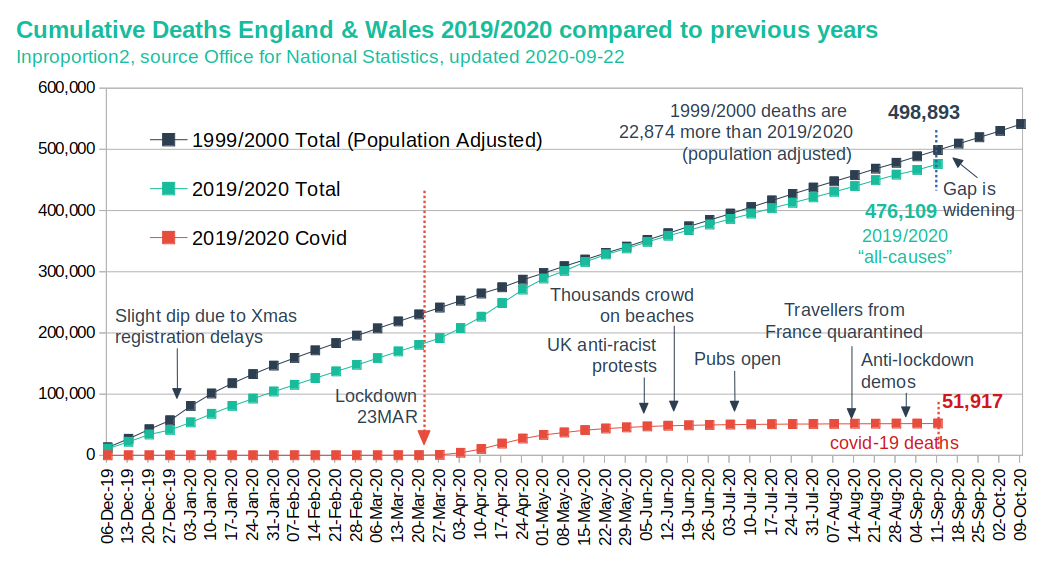
Sweden (no lockdown) and Britain (strict lockdown) have comparable disease and mortality statistics
US states with and without lockdowns have comparable disease and mortality statistics
Health
Hospitals remain empty and some face bankruptcy
Populations have T-cell immunity from previous influenza waves
Herd immunity needs only 15-25% population infection and is already achieved
Only when a person has symptoms can an infection be contagious
Tests:
Many scientists call this a PCR-test pandemic, not a corona pandemic
Very healthy and non-infectious people may test positive
Likelihood of false-positives is 89-94% or near certainty
Prof. Drosten developed his PCR test from an old SARS virus without ever having seen the real Wuhan virus from China
The PCR test is not based on scientific facts with respect to infections
PCR tests are useless for the detection of infections
A positive PCR test does not mean an infection is present or that an intact virus has been found
Amplification of samples over 35 cycles is unreliable but WHO recommended 45 cycles
https://www.globalresearch.ca/video-crimes-against-humanity-the-german-corona-investigation/5725795
The Great Barrington Declaration
The Great Barrington Declaration – As infectious disease epidemiologists and public health scientists we have grave concerns about the damaging physical and mental health impacts of the prevailing COVID-19 policies, and recommend an approach we call Focused Protection.
Coming from both the left and right, and around the world, we have devoted our careers to protecting people. Current lockdown policies are producing devastating effects on short and long-term public health. The results (to name a few) include lower childhood vaccination rates, worsening cardiovascular disease outcomes, fewer cancer screenings and deteriorating mental health – leading to greater excess mortality in years to come, with the working class and younger members of society carrying the heaviest burden. Keeping students out of school is a grave injustice.
Keeping these measures in place until a vaccine is available will cause irreparable damage, with the underprivileged disproportionately harmed.
Fortunately, our understanding of the virus is growing. We know that vulnerability to death from COVID-19 is more than a thousand-fold higher in the old and infirm than the young. Indeed, for children, COVID-19 is less dangerous than many other harms, including influenza.
As immunity builds in the population, the risk of infection to all – including the vulnerable – falls. We know that all populations will eventually reach herd immunity – i.e. the point at which the rate of new infections is stable – and that this can be assisted by (but is not dependent upon) a vaccine. Our goal should therefore be to minimize mortality and social harm until we reach herd immunity.
The most compassionate approach that balances the risks and benefits of reaching herd immunity, is to allow those who are at minimal risk of death to live their lives normally to build up immunity to the virus through natural infection, while better protecting those who are at highest risk. We call this Focused Protection.
Adopting measures to protect the vulnerable should be the central aim of public health responses to COVID-19. By way of example, nursing homes should use staff with acquired immunity and perform frequent PCR testing of other staff and all visitors. Staff rotation should be minimized. Retired people living at home should have groceries and other essentials delivered to their home. When possible, they should meet family members outside rather than inside. A comprehensive and detailed list of measures, including approaches to multi-generational households, can be implemented, and is well within the scope and capability of public health professionals.
Those who are not vulnerable should immediately be allowed to resume life as normal. Simple hygiene measures, such as hand washing and staying home when sick should be practiced by everyone to reduce the herd immunity threshold. Schools and universities should be open for in-person teaching. Extracurricular activities, such as sports, should be resumed. Young low-risk adults should work normally, rather than from home. Restaurants and other businesses should open. Arts, music, sport and other cultural activities should resume. People who are more at risk may participate if they wish, while society as a whole enjoys the protection conferred upon the vulnerable by those who have built up herd immunity.
On October 4, 2020
https://gbdeclaration.org/
The two-hour virtual panel, which highlighted controversial scientists from Harvard and Stanford universities, spanned several themes the Governor has touched on over the half-year the pandemic has impacted Florida. The common thread throughout the talk was that lockdowns are detrimental and the role of herd immunity in society, a politically-charged concept.
“Everything we’ve heard here, for example, in treating age groups differently, makes complete sense,” said Michael Levitt, a professor of structural biology at Stanford. “The need to let young people interact with each other, both for social reasons and for herd immunity, makes perfectly good common sense. I think there should have been more of that.”
DeSantis backed the need for students to live their lives and stressed that the current skew of infections toward young Floridians is precisely what the state wanted.
“What helps the elderly is if the young take this very minimal risk and live normal life until there’s herd immunity, and then, when we have herd immunity, then the older people can also live more normal lives,” said Dr. Martin Kulldorff, a professor at Harvard Medical School
Mask mandates, in his view, don’t limit COVID-19 spread. Rather, they increase social strife.
Lockdowns, all three scientists present agreed, are more detrimental to public health than the benefits of closing schools, restaurants and beaches. Kulldorff pointed to public health problems such as fewer regular hospital visits and mental health concerns that arise with lockdowns.
“Do we really want zero COVID?” Bhattacharya said. “To get zero COVID, I don’t know if it’s even technically feasible, but we know that we’re going to have to destroy our society in order to get it. We’ll have to get rid of all of our freedoms, we’ll have to make sure that very few people interact with each other. It essentially is so high a cost that it’s not worth it.”
https://floridapolitics.com/archives/369647-herd-immunity-the-phrase-of-the-day-at-gov-desantiss-panel-of-scientists
Mandated lockdowns had little effect on the spread of the coronavirus. The charts below show the daily case curves for the United States as a whole and for thirteen U.S. states. As in almost every country, we consistently see a steep climb as the virus spreads, followed by a transition (marked by the gray circles) to a flatter curve. At some point, the curves always slope downward, though this wasn’t obvious for all states until the summer.
we see in this data not only a lack of evidence that lockdowns caused the curves to bend, but also evidence of the very early stages of herd immunity.
https://www.nationalreview.com/2020/10/stats-hold-a-surprise-lockdowns-may-have-had-little-effect-on-covid-19-spread/
"The only time we believe a lockdown is justified is to buy you time to reorganize, regroup, rebalance your resources, protect your health workers who are exhausted, but by and large we'd rather not do it." He pointed to regions where tourism has suffered, the effects on farmers, and poverty levels.
"We really do appeal to world leaders, stop using lockdown as your primary control method. Develop better systems, for doing it, work together and learn from each other, but remember lockdowns just have one consequence you must never ever belittle and that is making poor people an awful lot poorer."
https://spectator.us/lockdown-incredible-vanishing-world-health-organization/
https://www.newsweek.com/fact-check-trump-who-covid-lockdowns-1538540
Charts:

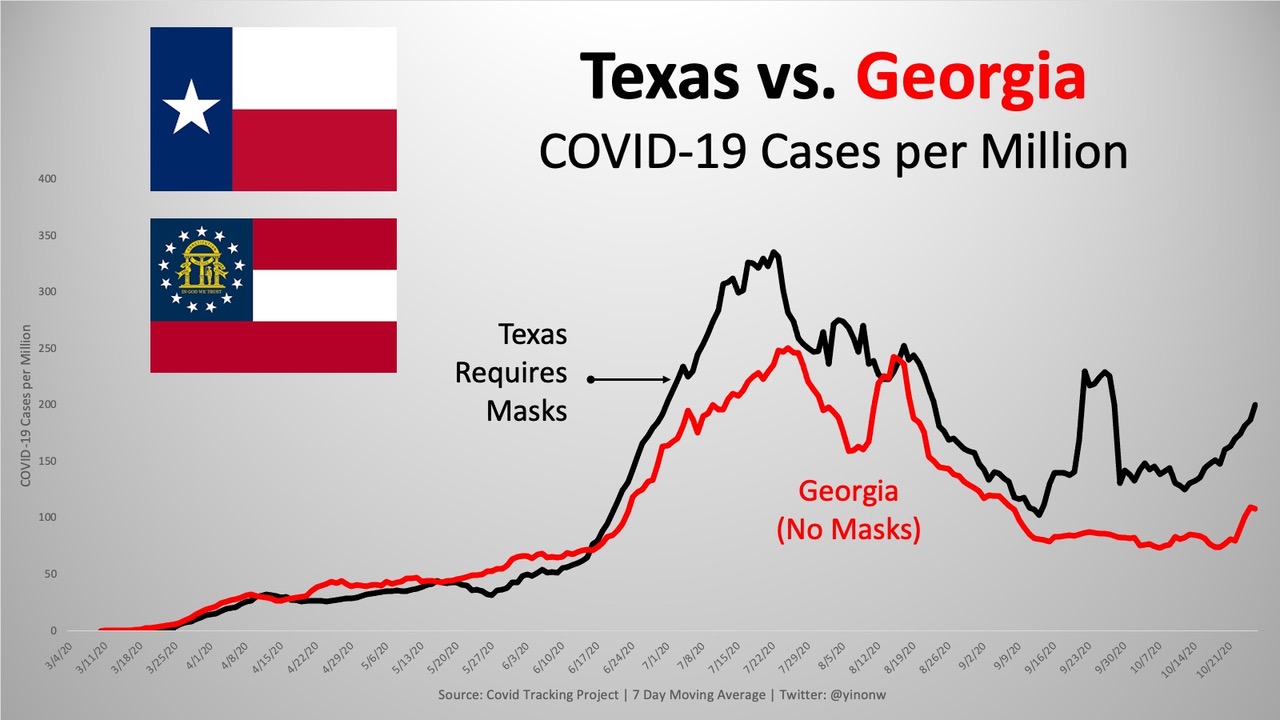
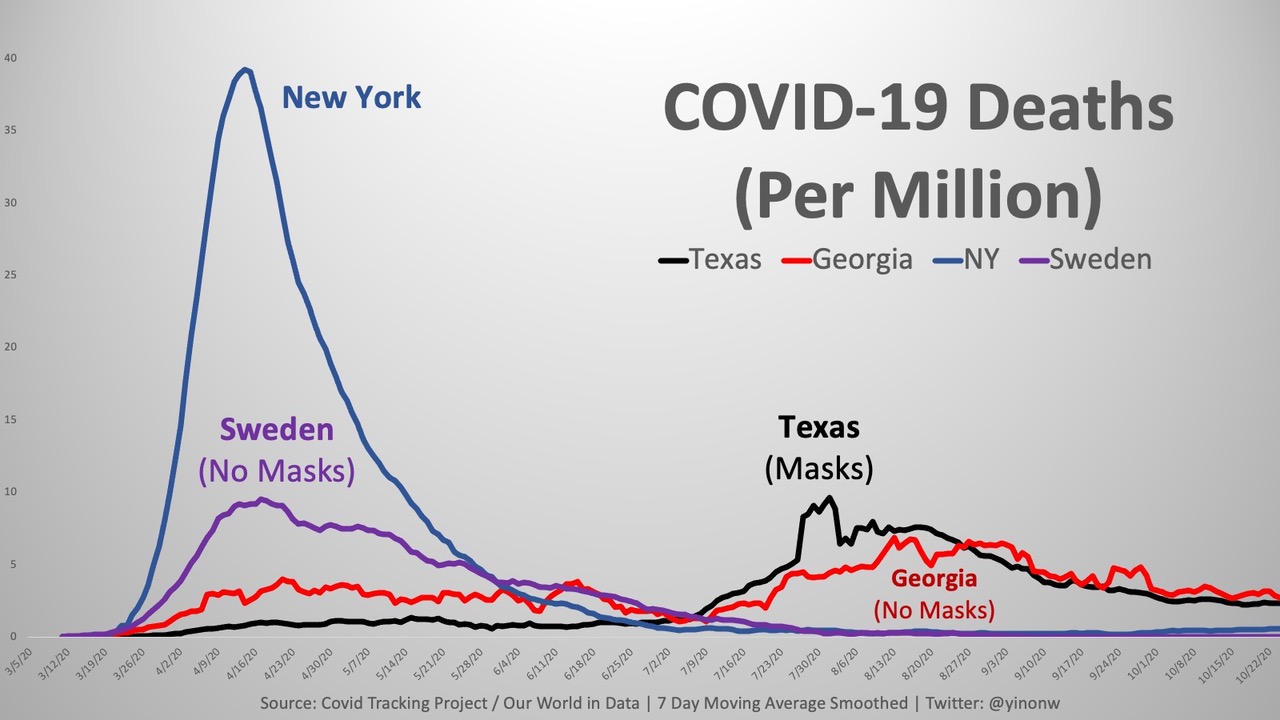
https://thefederalist.com/2020/10/29/these-12-graphs-show-mask-mandates-do-nothing-to-stop-covid/




https://rationalground.com/mask-charts/
Summary:
Facts about Covid-19
Updated: October 2020; Share on: Twitter / Facebook
Languages: CN, CZ, DE, EN, EO, ES, FR, GR, HE, HU, IT, KO, MS, NL, JP, PL, PT, RO, RU, SE, TR
Fully referenced facts about covid-19, provided by experts in the field, to help our readers make a realistic risk assessment. (Regular updates below).
“The only means to fight the plague is honesty.” (Albert Camus, 1947)
Overview
- Lethality: According to the latest immunological studies, the overall infection fatality rate (IFR) of covid-19 in the general population is about 0.1% to 0.5% in most countries, which is comparable to the medium influenza pandemics of 1957 and 1968.
- Treatment: For people at high risk or high exposure, early or prophylactic treatment is essential to prevent progression of the disease and avoid hospitalization.
- Age profile: The median age of covid deaths is over 80 years in most countries and only about 5% of the deceased had no serious preconditions. In contrast to pandemic influenza, the age and risk profile of covid mortality is thus comparable to normal mortality and increases it proportionally.
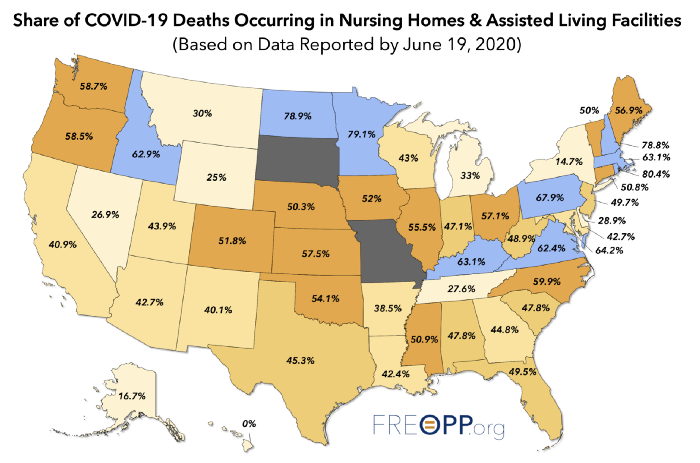
- Nursing homes: In many Western countries, up to two thirds of all covid deaths have occurred in nursing homes, which require targeted and humane protection. In some cases it is not clear whether the residents really died of covid or of weeks of stress and isolation.
- Excess mortality: Up to 30% of all additional deaths may have been caused not by covid, but by the effects of lockdowns, panic and fear. For example, the treatment of heart attacks and strokes decreased by up to 40% because many patients no longer dared to go to hospital.
- Antibodies: By summer 2020, global hotspots such as New York City and Bergamo had reached antibody levels of approximately 25%. Capital cities such as Madrid, London and Stockholm were around 15%. Large parts of Europe and the US, however, were still below 5%.
- Symptoms: Up to 40% of all infected persons show no symptoms, about 80% show at most mild symptoms, and about 95% show at most moderate symptoms and do not require hospitalization. Mild cases may be due to protective T-cells from earlier common cold coronavirus infections.
- Long covid: About 10% of symptomatic people report post-acute or long covid, i.e. symptoms that last for several weeks or months. This also affects younger and previously healthy people with a strong immune response. The post-viral syndrome is known from severe influenza, too.
- Transmission: According to current knowledge, the main routes of transmission of the virus are indoor aerosols and droplets produced when speaking or coughing, while outdoor aerosols as well as most object surfaces appear to play a minor role.
- Masks: There is still little to no scientific evidence for the effectiveness of cloth face masks in the general population, and the introduction of mandatory masks couldn’t contain or slow the epidemic in most countries. If used improperly, masks may increase the risk of infection.
- Children and schools: In contrast to influenza, the risk of disease and transmission in children is very low in the case of covid. There was and is therefore no medical reason for the closure of elementary schools or other measures specifically aimed at children.
- Contact tracing: A WHO study of 2019 on measures against influenza pandemics concluded that from a medical perspective, contact tracing is “not recommended in any circumstances”. Contact tracing apps on cell phones have also failed in most countries.
- PCR tests: The virus test kits used internationally may in some cases produce false positive and false negative results or react to non-infectious virus fragments from a previous infection. In this regard, the so-called cycle threshold or ct value is an important parameter.
- Medical mismanagement: In the US and some other countries, fatal medical mismanagement of some covid patients occurred due to questionable financial incentives and inappropriate protocols. In most countries, covid hospital mortality has since decreased significantly.
- Lockdowns: The WHO warned that lockdowns have caused a “terrible global catastrophe”. According to the UN, lockdowns may put the livelihood of 1.6 billion people at acute risk and may push an additional 150 million children into poverty. Unemployment, bankruptcies and psychological problems have reached record levels worldwide.
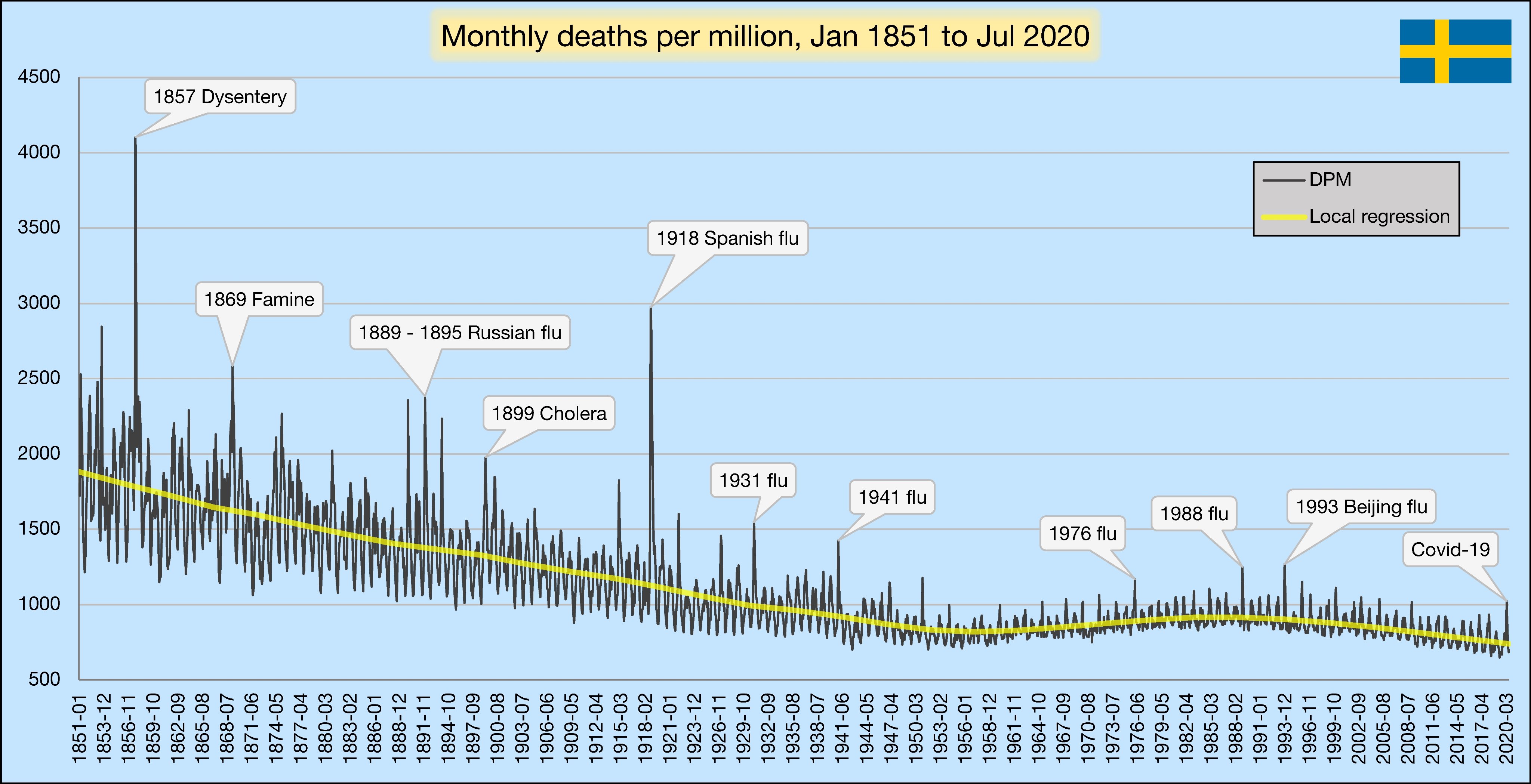
- Sweden: In Sweden, total mortality without lockdown has so far been in the range of a strong influenza season. 70% of Swedish deaths occurred in nursing homes that were not protected quickly enough. The median age of the Swedish covid deaths is 84 years.
- Media: The reporting of many media has been unprofessional, has maximized fear and panic in the population and has led to a massive overestimation of the lethality and mortality of covid. Some media even used manipulative pictures and videos to dramatize the situation.
- Vaccines: Several medical experts warned that express coronavirus vaccines may be risky. Indeed, the vaccine against the so-called swine flu of 2009, for example, led to cases of severe neurological damage and lawsuits in the millions. In the testing of new coronavirus vaccines, too, serious complications and failures have already been reported.
- Virus origin: The origin of the new corona virus remains unclear, but the best evidence currently points to a covid-like pneumonia incident in a Chinese mine in 2012, whose virus samples were collected, stored and researched by the Virology Institute in Wuhan (WIV).
- Surveillance: NSA whistleblower Edward Snowden warned that the covid pandemic may be used to permanently expand global surveillance. In several parts of the world, the population is being monitored by drones and facing serious police overreach during lockdowns.
https://swprs.org/facts-about-covid-19/